Connect With Us

Preventing Running Injuries
Over half of all runners encounter at least one injury per year. The reason for this is because many runners do not train properly. Injuries are almost inevitable due to the physical stress that running causes. While our bodies are great at adapting to the stress, it can only handle it in small doses. Injuries occur when the stress is applied too quickly for the body to handle, causing something within it to break down. With each step you take, your leg is absorbing two or three times your body’s weight.
Some of the most popular running injuries are shin splints, plantar fasciitis, Achilles tendinitis, and stress fractures. Shin splints cause pain along the inside or outside of the shins, and this pain is usually felt at the beginning of a run. The condition itself is defined as an inflammation of the muscles or tendons located around the shinbone. To treat shin splints, it is advised that you ice the shin area and stretch the calf muscles. To prevent this injury, you should slowly increase the distance you plan on running, instead of jumping into a more strenuous routine.
Achilles tendinitis is another common injury and it feels like pain along the back of the leg, toward the heel. This condition is defined as an inflammation of the Achilles which is the largest tendon in the body. The Achilles is responsible for connecting your calf muscles to the heel bone and it is caused by tight calf muscles. If you want to treat this injury, you should take a break from running to cross train with a low-impact activity.
There are a lot of common mistakes runners make that are causing them to experience injury. One mistake is stretching too much prior to warming up. If you plan to go on a run, you should warm up with a gentle 3-5-minute walk followed by a 5-minute run-walk. Another common mistake is jumping into a routine too quickly. Consequently, you should incorporate cross-training into your routine. If you are looking to get active, you should slowly weave running into an activity you are currently participating in. For example, you can try bike riding for 40 minutes followed by a 10-minute run.
Another way to prevent running injuries is to choose shoes that are appropriate for running. There are certain things you should look for when buying a new pair of running shoes. An important factor in these sneakers is flexibility. Running shoes should be capable of bending and flexing at the forefoot. However, you should not be able to bend the entire shoe in half with ease because this is a sign that the shoe does not have enough structure. Additionally, you should look for the fit of the running shoes you want to purchase. It is best to visit a specialty running shoe store to have your feet properly sized. Choosing shoes that fit properly can prevent many foot ailments.
If you are suffering from any pain from running injuries, you should make an appointment with your podiatrist to discover the underlying cause of your pain. He or she will be able to help treat your condition in the best way possible.
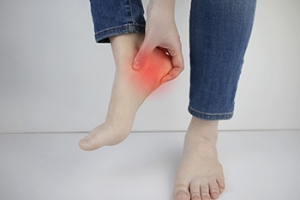
Heel Pain and Plantar Fasciitis

Heel pain, often attributed to plantar fasciitis, is a frequent complaint that affects individuals of all ages and activity levels. The plantar fascia, a thick band of tissue that supports the arch of the foot, can become inflamed and damaged, leading to persistent discomfort. Plantar fasciitis typically manifests as sharp, stabbing pain in the heel, particularly with the first steps in the morning or after long periods of rest. This pain often eases with activity but can return after periods of standing or walking. The condition is usually a result of repetitive strain, such as excessive use, which leads to micro-tears in the plantar fascia. Addressing heel pain and plantar fasciitis often involves a multi-faceted approach. Understanding the causes and treatment options for heel pain and plantar fasciitis is the first step in finding relief from this common, yet manageable, foot ailment. If you are experiencing persistent heel pain, it is suggested that you speak to a podiatrist who can determine the most appropriate approach to treating plantar fasciitis.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Boca Raton Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Boca Raton, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Prevention of Athlete’s Foot

Athlete's foot, medically known as tinea pedis, is a common fungal infection that affects the skin of the feet, particularly between the toes. It's caused by various types of fungi, including trichophyton and epidermophyton, which thrive in warm, damp environments such as sweaty socks or tight shoes. Athlete's foot often starts with itching and burning sensations, followed by red, flaky, or scaly skin, and sometimes is accompanied by blisters and a foul odor. To prevent athlete's foot, it is important to maintain exceptional foot health. Wash and thoroughly dry your feet daily, ensuring the spaces between your toes are clean and dry. Changing socks frequently, especially after physical activities, can also help. Opt for breathable footwear and avoid walking barefoot in public areas like locker rooms or swimming pools. By incorporating these practices into your routine, you can combat and prevent athlete's foot, maintaining healthy and happy feet. If you have developed athlete’s foot, it is strongly suggested that you are under the care of a podiatrist who can prescribe the right course of treatment for you.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Boca Raton Podiatry . Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Boca Raton, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Alternative Therapies for Non-Healing Diabetic Foot Ulcers

Maggot therapy, also known as Maggot Debridement Therapy, MDT, or Larval therapy, has a long history in medicine and has gained recent recognition for its unique ability to save limbs. This biotherapy involves placing disinfected maggots, often the larvae of the greenbottle blowfly, on wounds, such as diabetic foot ulcers, to debride necrotic tissues. It is particularly effective when antibiotics fail to combat bacterial infections in non-healing wounds, potentially preventing limb amputations. Maggots work by secreting special enzymes, which break down necrotic tissue, making it easier to digest and absorb. They also produce antibiotic-like agents and release ammonia to inhibit bacterial growth in the wound. Administration involves placing sterile maggots within a dressing on the wound for 48 to 72 hours. This therapy has broad applications, including diabetic ulcers, vascular ulcers, pressure ulcers, and even malignant wounds. Studies have shown that maggot therapy accelerates wound healing, reduces necrotic tissue, and decreases wound odor. While this therapy is highly effective, it should not be used for wounds near vital organs or blood vessels and in septic patients. Additional research can further expand the applications of this therapy, however, it saves 40 to 50 percent of limbs when used as a last resort. If you have a non-healing diabetic foot wound and would like alternative treatments for healing, it is suggested that you make an appointment with a podiatrist to discuss this further.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with one of our podiatrists from Boca Raton Podiatry . Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Boca Raton, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
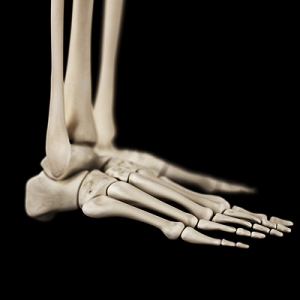
How Foot and Ankle Bones Harmonize for Stability

The human body is a marvel of engineering. This is evident in the biomechanics of the feet working together to maintain balance. Our feet consist of 26 bones and numerous ligaments and tendons that form a dynamic structure. At the foundation of this balance are the arches of the feet, formed by the interaction of these bones. The longitudinal arch runs along the length of the foot, while the transverse arch spans its width. These arches act like springs, absorbing shock and adapting to various surfaces. The ankle joint serves as a stabilizing pivot point. When we stand, walk, or run, our foot and ankle bones function as a cohesive unit, distributing our body weight evenly and absorbing the impact of each step. This can help us to adjust our posture and movements continuously. This intricate interplay of bones and joints allows us to navigate a wide range of terrains with grace and stability. It underscores the importance of caring for our feet and ankles, ensuring they remain in optimal condition for a lifetime of balanced mobility. If you would like more information about the interaction between foot and ankle bones, it is suggested that you consult with a podiatrist.
If you have any concerns about your feet, contact one of our podiatrists from Boca Raton Podiatry . Our doctors can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Boca Raton, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.